Page last updated: March 2026
The information on this webpage was adapted from Understanding Complementary Therapies - A guide for people with cancer, their families and friends (2026 edition). This webpage was last updated in March 2026.
Expert content reviewers:
This information is based on international and Australian research on complementary therapies. It was developed with help from a range of health professionals:
- A/Prof Geraldine McDonald, Director Patient Experience and Wellbeing, Peter MacCallum Cancer Centre, VIC
- Laura Carman, 13 11 20 Consultant, Cancer Council Victoria
- A/Prof Christine Carrington, Senior Consultant Pharmacist Cancer Services, Princess Alexandra Hospital and Metro South Health and The University of Queensland, QLD
- Kellie Giannarelli, Consumer
- Dr Suzanne Grant, Senior Research Fellow, Integrative Oncology, NICM Health Research Institute, Chris O’Brien Lifehouse, NSW
- Vivienne Hansen, Bush and Western Herbal Medicine Practitioner, WA
- Karla Jaji, Administration Officer, Nepean Cancer and Wellness Centre, NSW
- Dr Laura Kirsten, Senior Clinical Psychologist, Nepean Cancer Services, Nepean Blue Mountains Local Health District, NSW
- A/Prof Judith Lacey, Director of Supportive Care and Integrative Oncology, Chris O’Brien Lifehouse, NSW
- Adjunct Professor Danforn Lim, Western Sydney University and University of Technology Sydney, NSW
- Dr David Mizrahi, Senior Research Fellow and Accredited Exercise Physiologist, The Daffodil Centre, University of Sydney and Cancer Council NSW
- Professor Avni Sali AM, Founder and Director, National Institute of Integrative Medicine, VIC
- Gillian Thompson, Consumer
- A/Prof Kate Webber, Medical Oncologist, Monash Health, VIC
- Tanya Wells, Integrative Oncology Consultant and Naturopath, Melbourne Integrative Oncology Group, VIC
- Prof Kate White, Professor Cancer Nursing, Cancer Care Research Unit, The Daffodil Centre, University of Sydney and Cancer Council NSW
This page provides a brief overview of complementary and other therapies commonly used alongside conventional cancer treatments – listed in alphabetical order.
You will also find information about looking after your mental health through counselling or seeing a psychologist, which is part of conventional evidence-based treatment.
There is also information about medical systems or therapies yet to be studied. See Safety concerns and talk to your doctors and complementary therapists about which therapies are suitable for you.
Acupuncture
Acupuncturists put fine, sterile needles into certain points just under the skin. According to traditional Chinese medicine, qi (vital energy) flows through the body in channels called meridians.
Placing needles along these meridians is said to unblock and move qi, helping to reduce physical and emotional symptoms.
Research suggests that the needles stimulate the nervous system and the connective tissue in the body and help the body produce certain biomolecules such as hormones.
What to expect
After a consultation, which may include tongue and pulse analysis, the practitioner gently positions sterile needles into acupuncture points on your body.
The needles are left in place for 30 seconds to 30 minutes and may be stimulated manually by twirling or by using a machine (called electro-acupuncture). You may feel a tingling or dull ache, but it shouldn’t be painful.
Some acupuncturists use:
- press needles – small labels that stay in place for several days
- laser acupuncture – using laser light to stimulate acupuncture points.
Some people may bruise or bleed around the insertion point.
Check with your doctor whether acupuncture is suitable for you, as penetration of the skin barrier by needles may increase the risk of infection or bleeding for some people having cancer treatment.
For more about what to expect during an acupuncture session, visit Chinese Medicine Board of Australia.
Evidence
International clinical guidelines recommend acupuncture for:
- joint pain related to using aromatase inhibitors
- an option for managing cancer pain and musculoskeletal pain
- tingling in the hands and feet from chemotherapy (peripheral neuropathy)
- cancer-related fatigue, and
- hot flushes.
Evidence also suggests that acupuncture may help with nausea and vomiting caused by chemotherapy, with trouble sleeping and with anxiety. It is not clear whether it helps relieve dry mouth, but several studies are underway.
In Australia, use of the term acupuncturist is regulated by the Australian Health Practitioner Regulation Agency (Ahpra) and the Chinese Medicine Board of Australia (CMBA).
To check whether your acupuncturist is registered, visit Ahpra. Some registered acupuncturists have special training in treating cancer-related conditions. Ask your doctor whether acupuncture is offered at your treatment centre.
Aromatherapy
This is the use of essential oils extracted from plants. The oils are used mainly during massage but can also be used in a bath or an oil burner (sometimes called a diffuser or vaporiser).
When inhaled or absorbed through the skin, the oils are thought to have a positive effect on the body’s tissues, the mind and spirit.
What to expect
The aromatherapist blends essential oils and adds them to a base (carrier) oil before applying them to your skin during a massage.
Evidence
There is some limited evidence that aromatherapy may have positive short-term effects on pain and anxiety in people with cancer.
There is some small evidence that aromatherapy improves sleep and quality of life.
Safety of essential oils
Essential oils are concentrated oils that are extracted from plants, such as lavender or tea tree. They are very strong, so they must be diluted with a base oil before using on your skin.
Base (or carrier) oils are usually made from kernels or nuts, such as almonds, or sometimes castor oil. Sometimes mineral oil is used instead as it is odourless.
These oils should never be used inside the body (e.g. taken in a drink or swallowed). Also take care not to touch your eyes if some oil gets on your hands.
Allergic reactions to oils are rare, but some people find they irritate the skin, or the smell makes them feel nauseous or gives them a headache.
Let your therapist know if you have had reactions to oils in the past, or if you don’t like certain smells.
Art therapy
The process of creating art can be a way to express feelings and explore issues that may be hard to put into words. Talking about the work that you create with a trained art therapist can help you better understand your emotions and concerns.
What to expect
With the support of an art therapist, you can create any type of art: drawing, painting, collage, sculpture or digital work. Some cancer centres run art therapy programs.
Art therapy may be done individually or in a group. You don’t need to be “good” at art. The focus is on the process of making artwork, not the result.
Evidence
There is some evidence art therapy can help with symptoms of fatigue, anxiety, depression and improve quality of life.
Anecdotal reports suggest it improves coping skills and emotional wellbeing.
What is Ayurvedic medicine?
This is an ancient Indian system. Ayurveda is from the Sanskrit words ayur (life) and veda (knowledge).
Key concepts
- Health is achieved when the mind, body and spirit are in balance.
- Every person is a combination of five elements: air, water, fire, earth and space.
- These elements combine to form three energies or life forces called doshas: vata, kapha and pitta.
What to expect
The practitioner will ask about your lifestyle, diet, emotional wellbeing and medical history. They will look at your tongue and take your pulse.
All this information is used to assess what Ayurveda calls your vital force and overall balance in the body.
Suggested treatments vary from person to person, and may include herbal medicine, dietary changes, massage, meditation and yoga.
Chinese medicine
Chinese medicine is based on the idea of maintaining balance between the mind, body and environment to prevent and manage diseases. It focuses on the person’s overall condition, not just their symptoms.
There are different Chinese medicine practices, including acupuncture; breathing and movement exercises called qi gong; movement exercises called tai chi; the practice of burning herbs near the skin called moxibustion; herbal medicine; and Chinese dietary therapy or food therapy (what you eat).
Key concepts
Qi
According to Chinese medicine, everyone has a vital energy or force in the body known as qi (pronounced “chee”).
When you are healthy, qi flows easily through the body’s meridians (channels). If the flow of qi becomes blocked, the body’s harmony and balance is affected, causing disease.
Yin and Yang
Qi is made up of two opposite but complementary forces known as Yin, represented by water, and Yang, by fire.
Yin and Yang are believed to be in everything and the balance between them maintains harmony in your body, mind and the universe.
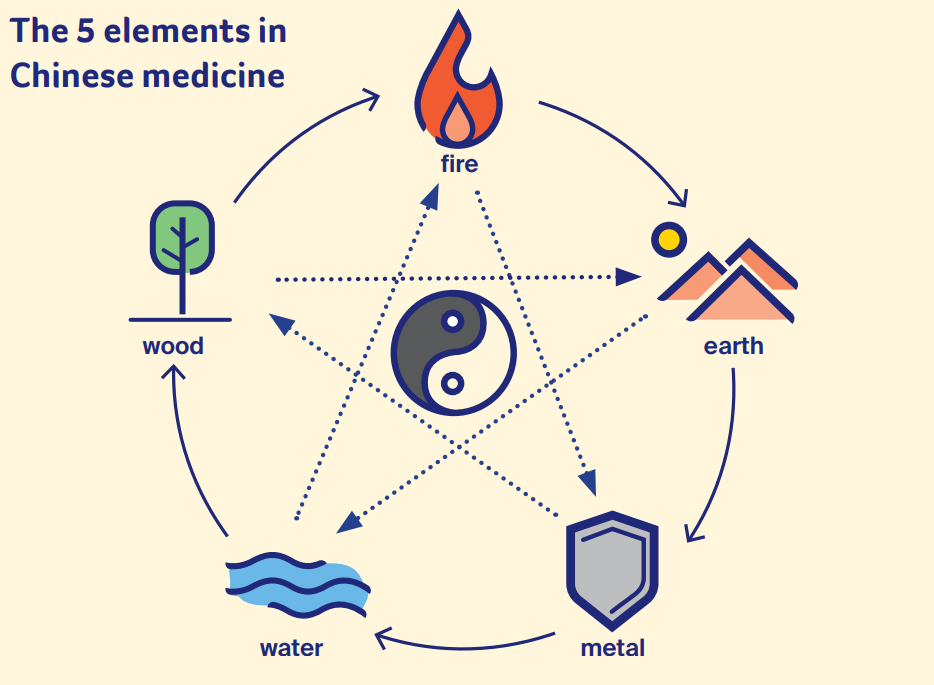
Elements
Chinese medicine uses the theory of 5 elements – fire, earth, metal, water and wood. These elements relate to particular organs and tissues in the body.
What to expect
A practitioner will ask you questions and do a physical examination, which may include looking at your tongue and taking your pulse. Treatment is individual and may include a combination of therapies.
To learn more about what Chinese medicine is and what to expect during a Chinese medicine consultation, visit the Chinese Medicine Board of Australia’s (CMBA) website.
Chinese herbal medicine
In Chinese herbal medicine, various parts of certain plants (such as leaves, roots, stems, flowers and seeds) are used as medicine, based on the belief that they can influence meridians and help restore balance in the body.
What to expect
A practitioner will choose a combination of herbs and foods with the aim of bringing your body back into balance.
They may make a formula tailored to you, or dispense herbal medicines pre-packaged as granules, pills or raw herbs to be made into a tea.
Evidence
Many Chinese herbs have been scientifically evaluated for how well they work for people with cancer. Studies have found benefits for some herbs. For example, American ginseng has shown benefits for cancer-related fatigue.
Research is continuing to examine the benefits of different herbs and different herbal combinations.
Safety
Chinese herbal medicine is a complex area and you should see a registered Chinese medicine practitioner rather than treating yourself.
See Safety concerns for tips on using herbs and visit Ahpra to check your practitioner is registered with the Chinese Medicine Board of Australia.
Counselling
Talking with a counsellor or psychologist can help you identify goals you would like to achieve, develop ways to deal with difficult situations or relationships in your life, and look at how to manage your feelings.
Counselling allows you to explore ways of resolving negative thoughts and feelings that may affect your health and day-to-day life. Counselling provides a safe, supportive and confidential environment to learn new coping skills.
It can strengthen your ability to deal with challenges, and help you learn new ways of looking at your life choices and behaviours. Some people find it easier to express their emotions to a counsellor than with someone they know.
You can talk about thoughts and feelings that you might not feel comfortable sharing with your family and friends. Counselling may also give you strategies to manage fear of the cancer coming back (recurrence). This can be helpful after treatment ends.
What to expect
Sessions may be face-to-face, over the phone or online. There are different types including cognitive behaviour therapy (CBT), grief therapy, life coaching, acceptance and commitment therapy, and person-centred therapy.
Ask the therapist about their approach to see if it suits you. Counselling can be for you, or for family and friends affected by cancer.
Evidence
There is strong evidence that counselling can help to manage distress, fear and can improve quality of life.
There is good evidence that psychological therapies such as CBT can help reduce a range of concerns, including anxiety and depression, cancer-related fatigue and insomnia.
Specific therapies (including CBT) for managing the fear of recurrence have shown some benefits.
Who can help with emotions
If you would like to talk to someone or need emotional support there are a variety of health professionals and services that can help.
It’s important to find someone who is suitably qualified and who you feel comfortable talking with.
Let them know if you have a history of anxiety, depression or other mental health concerns, as you may be feeling more vulnerable during this time.
Psychologist
Psychologists use evidence-based strategies to guide people through issues with how they think, feel and learn. They cannot prescribe medicines.
To be registered with Ahpra, a psychologist must complete four years of psychology at undergraduate level, followed by postgraduate study and ongoing continuing professional development.
Counsellor
Counsellors help people develop strategies to manage their concerns. They don’t need any qualifications to practise, though many counsellors have qualifications in counselling, nursing, social work or psychology.
It’s a good idea to check their qualifications before making an appointment. Counselling may be available through your local Cancer Council – call 13 11 20. Beyond Blue offers free counselling.
Psychiatrist
Psychiatrists are trained and Ahpra-registered medical doctors who specialise in the diagnosis, treatment and prevention of mental illness.
They can prescribe medicines to help manage a range of mental and emotional conditions.
How to find a mental health professional
Ask your GP for a referral – you may be eligible for a Medicare rebate. To find a psychologist near you, visit the Australian Psychological Society. To find a psychiatrist, visit Your Health in Mind.
You may be able to see a psychologist or psychiatrist at your hospital or cancer treatment centre.
Online self-help programs or smartphone apps can help you track how you’re feeling. Many are free to download. Visit moodgym or MindSpot.
For 24-hour crisis support, call Lifeline on 13 11 14.
Flower remedies
Also called flower essences, these are highly diluted extracts made from the flowers of wild plants.
There are many types from around the world, including the Original Bach Flower Remedies, developed in England in the 1930s, and Australian Bush Flower Essences, developed in Australia in the 1980s.
They may be used by a flower essence practitioner, some naturopaths, herbalists or other complementary therapists. Some people believe that flower remedies balance the mind, body and spirit, and help you cope with emotional issues.
What to expect
Similar to a counselling session, you may be asked about problems you’re having and how you feel about or respond to certain situations.
The therapist may suggest a single essence for you. Or they may prepare a blend of essences (remedy) that is tailored specifically for you. You then take the essence, usually in water, several times a day.
Always check what’s in the remedy (the name may not include the ingredients) and discuss with your cancer care team before taking it.
Some herbs may interact with some cancer treatments and medicines, and cause side effects. See Safety concerns for tips on using herbs safely.
Evidence
Scientific evidence does not support the use of flower remedies for treating diseases. However, anecdotal reports suggest they may help reduce fear and distress.
“After surgery, my naturopath gave me Bach Flower Remedies for fear, shock and exhaustion. These helped me relax.” Louise
Healing touch
This is the placement of hands in specific sequences above or on the body to detect temperature, texture or what are called vibration changes, which practitioners believe indicate areas of energy imbalance.
Healing touch claims to work with your personal energy field to support the body’s own natural ability to heal.
What to expect
Healing touch can be done while you are sitting, lying down or standing. The therapist may perform a meditation and then move their hands over your body.
Evidence
There is no scientific evidence of energy fields or that healing touch has any medical benefit. Some people find healing touch relaxing.
What is homeopathy?
Homeopathy uses plant, mineral and animal substances – highly diluted in water – as remedies.
Key concepts
It is based on the theory that “like cures like” and that remedies stimulate energy in the body to relieve symptoms, restore vitality and reduce emotional imbalances.
What to expect
The homeopath asks about your medical history, and considers how you respond physically and emotionally to your symptoms. They may prescribe a remedy as liquid drops, tablets or a skin cream.
Evidence
There is no reliable scientific evidence that homeopathy works. Most remedies are so diluted they are likely non-toxic.
But some products, especially if bought online or overseas, may contain active substances, heavy metals or harmful contaminants.
There are reports of serious side effects from certain homeopathic preparations. Only use products regulated by the TGA and discuss it with your care team first.
Hypnotherapy
Hypnotherapy uses deep relaxation to help people become aware of their inner thoughts and find ways to manage them.
It may help improve mental wellbeing and overcome mental blocks around anxiety, fear, low self-esteem, pain, insomnia and unwanted habits such as smoking.
What to expect
A trained therapist will ask you about your current health and medical history and discuss your reasons for having hypnotherapy.
They will then guide you into a deeply relaxed state, known as an altered state of consciousness.
In this relaxed state, your subconscious can focus on your treatment goals, making them more achievable for your conscious mind.
Evidence
Clinical studies show that hypnotherapy can help people cope with pain, anxiety, fatigue, hot flushes and nausea and vomiting related to cancer treatment.
Light and temperature therapies
Research into light therapy you can do at home or at a spa is limited, but suggests it may be okay in some specific situations (e.g. for oral mucositis, some pain or for lymphoedema).
But it hasn’t been shown to be generally safe for people with cancer. There is particular concern about using red light therapy over tumour sites. Talk to your doctor about light therapy, even if you’ve used it before.
Some hot or cold therapies claim to help with circulation, scarring, sleep or immune function. But saunas and steam rooms may be dangerous for people with heart concerns.
Your treatment team may offer cold therapy during chemotherapy to reduce the chance of peripheral neuropathy (tingling in hands/feet), but other cold therapies might not be suitable.
Check with your doctor before trying heat or cold therapies.
Massage
Massage involves moving (manipulating) muscles and rubbing or stroking soft tissues to promote relaxation. By applying pressure to muscles and pressure points, massage helps to release both muscular and emotional tension.
Oncology massage therapists are specially trained to adjust pressure, speed, duration and direction of strokes to provide a safe session for a person with cancer.
The style of massage used will depend on the treatment you’re having. It may be helpful at any stage, from those newly diagnosed, to people who have finished their cancer treatment.
There is no evidence that massage can increase the risk of cancer cells spreading to other parts of the body.
A type of massage called manual lymphatic drainage can help reduce the symptoms of lymphoedema (swelling caused by a build-up of lymph fluid).
What to expect
Massage is usually done in a warm, quiet room while you lie on a massage table or sit in a chair. The therapist uses a variety of strokes on different parts of the body.
In people with cancer, therapists may adjust their pressure and avoid certain areas of the body.
Some styles of massage are done with you fully clothed; others require you to undress to your underwear so the therapist can use oil to move their hands over your skin more easily.
The therapist may place pillows under different parts of your body for support. Let the therapist know if you need a change in pressure or a blanket.
Evidence
Many scientific studies have shown that oncology massage may help manage stress, anxiety, pain, depression, fatigue and insomnia in people who have had chemotherapy or surgery for cancer.
Massage safety for people with cancer
Chemotherapy
This drug treatment affects the whole body. If you have a chemotherapy port, massage should not be done in this area.
Some people who have chemotherapy have tingling in their hands or feet (peripheral neuropathy), or may find they bruise or bleed easily, so need to avoid deep massage.
Radiation therapy
The skin may be sensitive, red and appear sunburnt after external radiation therapy.
Avoid massage to the treated area once any skin changes appear or your skin becomes sensitive. Massage oils, especially ones with fragrance or essential oils, may make already irritated skin feel worse.
Surgery
Recovery takes time. It’s important to avoid massaging the surgical area until wounds have healed and there are no complications such as blood clots, infections or trapped pockets of fluid under the skin (seroma).
Ask your surgeon when it is safe to start scar massage after surgery.
Bone fragility
Radiation therapy, medicines or the cancer itself may make bones more fragile. Care should be taken to avoid applying too much pressure.
Risk of lymphoedema
Radiation therapy or lymph node removal in the neck, armpit or groin can increase your risk of lymphoedema. See a trained lymphoedema therapist.
If you already have lymphoedema, manual lymphatic drainage from a trained therapist may help. Visit the Australasian Lymphology Association to find a registered practitioner
Medicinal cannabis
Some people want to find out about using cannabis for medical purposes. Cannabis is a plant that contains chemicals called cannabinoids, which act on certain receptors found on cells in our body.
Cannabinoids can also be made in a laboratory. Medicinal cannabis contains standard amounts of cannabinoids.
Two cannabinoids commonly used in medicinal cannabis are delta-9-tetrahydrocannabinol (THC) and cannabidiol (CBD).
Evidence
There is no evidence that medicinal cannabis can treat or cure cancer. Research studies have looked at the potential benefits of using medicinal cannabis to relieve cancer symptoms and treatment side effects.
There is some evidence it may help people with certain symptoms and side effects (e.g. nausea and vomiting caused by chemotherapy) if conventional nausea treatment doesn’t work.
To date, published studies have shown medicinal cannabis to have little effect on appetite, weight, pain or sleep problems. Research is continuing in these areas.
Legal access
Medicinal cannabis is legal in Australia when prescribed by a medical practitioner registered to prescribe it.
Most medicinal cannabis products in Australia are unapproved, meaning that your doctor must get approval from the government before prescribing.
If your doctor doesn’t prescribe medicinal cannabis, they may still support your decision to use it, so tell them if you get a cannabis prescription elsewhere.
The laws about access to medicinal cannabis vary in each state and territory, which may affect whether it can be prescribed for you.
The TGA allows low-dose CBD products (up to 150 mg of CBD a day) to be listed on the Australian Register of Therapeutic Goods (ARTG) and sold over the counter by pharmacists.
At the time of publication (December 2025), no product has been approved via this pathway.
Medicinal cannabis may interact with some medicines and affect your driving. Visit the TGA for information.
Mindfulness
Mindfulness is the practice of being fully present and engaged in the moment — free from distraction or judgement.
Common mindfulness practices can include focusing on the breath and observing each rise and fall, body scan meditations, and mindful walking.
Mindfulness based stress reduction (MBSR) is a 6–8 week course designed to help you cope better and feel more at ease in your life. People practise mindfulness to change the way they think about experiences.
By becoming aware of thoughts and feelings, you can choose how to handle them in the moment. This can improve attention and awareness, and strengthen wellbeing.
What to expect
Mindfulness can be practised sitting, standing or lying down. An instructor will support you to focus attention in a mindful way.
This could be through following a series of exercises that focus on breathwork and calming the mind.
Evidence
There is good evidence to show that MBSR can lower the levels of stress hormones in your body, which can assist in healing and improve immune function.
Clinical practice guidelines include MBSR as an option for managing cancer-related fatigue.
Studies on mindfulness show it helps improve the quality of life of people with cancer, increases coping, and can reduce pain, anxiety, depression and nausea.
“Even 13 years after I was treated for cancer, in the back of my mind I still worry that it will come back. I did a mindfulness course to help me deal with this fear and found it really helpful.” John
Music therapy
Music therapy may help people express themselves, feel more in control and hopeful, focus on healing, feel less anxious, connect with others and simply enjoy the moment.
What to expect
You don’t need to be musical to take part or benefit. The structure of the session depends on the needs of the participants and what you feel comfortable with.
You may play instruments, sing, write lyrics, or listen to music and discuss how it affects you. Music therapy may be done in a group or one-on-one with a therapist.
Evidence
Some evidence-based studies show music therapy can improve anxiety, depression, fatigue and quality of life in people with cancer.
What is naturopathy?
Naturopathy focuses on the foods you eat, and your individual health, wellbeing and nutrition needs.
Key concepts
- Good health depends on the connection between the mind, body and spirit.
- The body has the ability to heal.
- Based on six principles: use the healing power of nature; find and treat the causes; first do no harm; doctor as teacher; treat the whole person; focus on prevention.
What to expect
After asking about your health, a naturopath may suggest changes to your diet, more time in nature (e.g. water and sunlight), massage or exercise, lifestyle changes, counselling, and herbal or nutritional remedies.
A naturopathic nutritionist gives advice on diet using nutrient rich whole foods. They recommend avoiding artificial flavours, chemicals and other additives.
You may be prescribed specific herbs or supplements.
Qi gong
Qi gong – pronounced “chee goong” – is part of Chinese medicine. “Qi” means vital energy and “gong” means work. Qi gong combines movement with controlled breathing and meditation.
It may be considered both a body-based practice and an energy therapy. In Chinese medicine, movements performed in qi gong are believed to keep the flow of energy running through the body’s energy channels.
This is said to help improve quality of life, including mental and physical wellbeing.
What to expect
Wear comfortable clothes. The session starts with warm-up exercises to loosen the body. The instructor then guides you through a series of slow movements, to help you become more aware of your energy.
Classes may also include meditation while lying down, sitting, standing or walking.
Evidence
Clinical studies suggest that qi gong improves quality of life and reduces fatigue, pain and anxiety. Anecdotal reports suggest that it helps improve general fitness.
Reflexology
Reflexology is a type of foot and hand massage based on the belief that areas on the feet and hands, called “reflex points”, correspond to the body’s internal organs and systems, like a map.
Practitioners believe that pressing on reflex points can unblock energy pathways (meridians) and promote health in the related area of the body.
What to expect
After discussing your health and concerns, you take off your shoes. While you are sitting or lying down, the reflexologist works with their hands on your bare feet, possibly using cream or oil.
Many people find it relaxing, like a massage, although sometimes certain parts of the hand or foot may feel tender or painful.
Some cancer treatments (e.g. taxanes, capecitabine) can cause sore skin on the feet and weak nails. In this case you should avoid reflexology.
Evidence
Some clinical practice guidelines include reflexology as an option for managing chemotherapy side effects such as pain and peripheral neuropathy (tingling in the hands and feet).
Several clinical trials have looked at using reflexology for anxiety, fatigue, breathlessness and quality of life.
However, studies have involved small groups, so it’s difficult to say whether the reflexology had any effect.
Reiki
The term reiki is a Japanese word meaning universal life energy. It is a gentle hands-on therapy that is based on the belief that therapists can channel healing energy into another person to promote health.
Some people use reiki because they believe it improves physical, emotional and spiritual wellbeing.
What to expect
During a reiki session, you sit or lie down fully clothed. The therapist places their hands in a series of positions on or slightly above your body. The aim is to promote wellbeing.
Evidence
There is no reliable scientific evidence that reiki has any benefits.
Anecdotal reports suggest that reiki may be calming and relaxing for some people, and other anecdotal reports claim that it may be helpful in relieving pain and anxiety, reducing stiffness and improving posture.
Relaxation and meditation
Relaxation is a process that uses slow breathing and muscle-loosening exercises to physically and mentally calm the body.
Techniques include progressive muscle relaxation, guided imagery, deep breathing, massage, aromatherapy and yoga.
Meditation is the practice of focusing awareness and attention on the present moment and on the senses of the body. It is an important part of many religions, including Buddhism and Hinduism, but you don’t have to be religious to meditate.
There are different types of meditation techniques, including breathwork. Relaxation and meditation may help to release muscle tension, reduce anxiety and depression, and help improve quality of life.
They may be used to help calm and relax the body and mind. Your hospital or cancer support group may offer relaxation and meditation groups.
Self-help podcasts, online videos and smartphone apps can also guide you through the techniques. You can also try our free relaxation and meditation podcast Finding Calm During Cancer.
What to expect
Serene music may be played to create a peaceful environment. The therapist will guide you through exercises to help you learn the skills of relaxation and meditation, which you can then practise at home.
Guided imagery uses sound and visual prompts to encourage your imagination to create pleasant thoughts.
After a period of relaxation, you will usually be prompted to stay awake and enjoy your relaxed state of mind. Relaxation and meditation can be done sitting or lying down.
Evidence
Clinical practice guidelines include offering a combination of guided imagery and progressive muscle relaxation for people experiencing pain after cancer treatment.
Clinical studies have shown that people being treated for cancer who practise relaxation often have lower levels of anxiety, stress, pain and depression.
Relaxation techniques have also been shown to improve sleep.
Sound therapy
Sound therapy, also known as sound healing, uses vibrational music or instruments such as Tibetan singing bowls, gongs and tuning forks to create different sound frequencies.
Singing bowls are usually made from crystal, but may sometimes be brass, glass or metal. Their size varies, and they can be quite large, with different sizes creating different “notes” and vibrations.
Sound therapy is often practised as a “sound bath” or “frequency healing” where your body is surrounded by soothing sounds designed to induce relaxation and healing.
The vibrations and sound frequencies produced during sound therapy are believed to reduce stress and help balance emotions. It’s a gentle, non-invasive therapy that may help anxiety, fatigue and tension.
What to expect
In a typical session, you’ll lie down comfortably while a practitioner plays instruments like singing bowls or gongs – often close to your body.
Sometimes centres may offer sessions using recorded “frequency” music. The sounds and vibrations surround you and may encourage deep relaxation.
Evidence
Scientific studies show that sound therapy may help with anxiety and depression, improve sleep and reduce fatigue. Research also suggests that it may promote relaxation and stress relief.
Spiritual practices
Spirituality is a very individual concept. For some people, it may mean being part of an organised religion such as Christianity, Judaism, Islam, Buddhism or connecting deeply to culture.
For others, spirituality may reflect their individual beliefs about the universe and their place in it, or a search for meaning and purpose in their lives.
When people are diagnosed with cancer, the spiritual aspect of their lives often becomes more important. People may find comfort in prayer, meditation or quiet contemplation.
Receiving care from a spiritual care practitioner, who may be called a pastoral carer, chaplain or priest, can help people – even those who are not part of an organised religion.
What to expect
If you are part of a spiritual or religious community, you may benefit from:
- prayer or meditation groups
- a feeling of unity and connection with the congregation
- practical, emotional and spiritual support offered by members of your spiritual or religious community.
If you are not part of a formal community, you can find out more about your area of spiritual interest from a spiritual care practitioner, support groups, friendship groups, your local library or online.
A spiritual care practitioner is often a member of the team at hospitals and cancer treatment centres.
Evidence
There’s growing scientific evidence of a positive link between spiritual practice and health.
It has been shown to reduce stress, instil a sense of peace and improve the ability to manage challenges.
Tai chi
A part of Chinese medicine, tai chi combines gentle movement, deep breathing techniques and meditation. The movements create stability in the body, reflecting the ancient Chinese concept of balance known as Yin and Yang.
The breathwork of tai chi is calming and meditative. Creating and holding the poses helps to loosen and strengthen muscles. Tai chi can be modified for groups that are less mobile.
What to expect
During class there will be serene music playing. The class usually starts with warm-up exercises. You will be shown different moves and assisted to perform them.
The instructor may use names to describe the poses, for example, “white crane spreads its wings”. Movements start out simple and gradually get harder, with many parts of the body needing to move to achieve the pose.
The class ends with cooling down and relaxation.
Evidence
Studies have shown that tai chi can improve quality of life, balance, agility, flexibility and muscle tone in cancer survivors.
While there is less certainty, some studies suggest that tai chi may also help reduce fatigue, anxiety, depression and stress.
“I joined a tai chi class organised through the Carers Association and also attended their support workshops and relaxation sessions. The encouragement from other carers gave me the confidence boost I needed.” Isabella (carer)
Traditional healing practices
Some people use traditional healing practices as a complementary therapy. If you want to use traditional remedies from your culture alongside conventional medical treatment, ask your treatment team.
For Aboriginal and Torres Strait Islander peoples, healing is holistic. This mean that it includes the physical, emotional, spiritual and cultural aspects of wellbeing.
Many First Nations communities use bush medicine, sometimes called medijin or medijina. It can help to reconnect with land, culture and ancestors, and to bring peace of mind.
Bush medicines may include a smoking ceremony, something you put on your skin or plant remedies passed down through generations.
Safety and precautions
Bush medicines can be meaningful and supportive, but some may also interact with cancer treatments or interfere with medicines. It’s possible they may also cause side effects or affect your cancer treatment outcomes.
Although herbs and plants may be natural, they still need to be used with care. See Safety concerns for more on this.
Bush medicine is not a replacement for conventional medical treatment. Tell your health care team about traditional practices that you plan to try.
Being honest about what you want to try helps ensure your care is safe, respectful, and aligned with your values.
Accessing traditional therapies
If you want to use bush medicine, discuss this with a traditional healer, an Aboriginal Health Worker or an Elder. They can guide you on culturally safe practices and help you to communicate with other members of your medical team.
There are many nations and traditions amongst First Nations peoples, so therapies vary depending on whose country you live on. Try to connect with local health workers and providers to get the best knowledge and support.
Access traditional healing through:
- community healing centres (e.g. Akeyulerre in Alice Springs)
- Ngangkari healers, who offer spiritual and physical healing in some hospitals and clinics
- local Aboriginal Medical Services, which may provide bush medicine workshops or referrals.
Some common bush medicine plants
Gumbi gumbi
Traditionally used for colds, skin conditions, fatigue, digestion and emotional wellbeing. It’s taken as a tea or tonic.
Native lemongrass
Used for calming effects and to reduce pain. It may ease stress and discomfort during treatment.
Emu bush
Used in smoking ceremonies and on the skin for general wellbeing. Being studied in research.
Kakadu plum
Taken as a powder, supplement or eaten to help support general health during treatment. This fruit is very high in vitamin C and antioxidants.
You should avoid it if your doctor has said you should not take vitamin C supplements.
Maroon bush (Murrin murrin)
Traditionally used for infections, chronic illness and to support general health. Often taken as a tea.
It should not be taken without medical advice and needs a prescription in Western Australia.
Western herbal medicine
Herbal medicines are often used to help manage the side effects of conventional cancer treatments, such as reducing fatigue and improving wellbeing.
Evidence shows that they should only be used in addition to conventional medical treatment, rather than as an alternative therapy.
Using herbs is complex and it’s best to see an experienced practitioner rather than trying to treat yourself.
Some herbs may interact with conventional cancer treatment or medicines, and change how the treatment works or how the dose is absorbed. See pages Safety concerns for tips on using herbs safely.
What to expect
After asking you some questions, the practitioner puts together a holistic picture of your health.
They will look for underlying reasons for your ill health or symptoms, and provide a herbal mixture aimed at addressing the causes and symptoms of your illness.
The practitioner may give you a pre-made herbal formula, but more often they will prepare a blend of herbs specifically for your needs.
Herbal medicines can be prepared:
- as liquid extracts, usually taken with water
- as herbs that are made into a tea or infusion
- as creams applied to the body;
- or as tablets or capsules.
Western herbal medicines are usually made from herbs traditionally grown in Europe and North America, but some come from Asia.
Evidence
There is a wide body of research into the effectiveness and safety of many herbs, and some studies show promising results.
Speak to your doctor, pharmacist and herbal medicine practitioner about the potential benefits and side effects of any herbal preparations.
Yoga
Yoga can increase physical activity and improve emotional health. It involves holding postures (asanas) with the body, being aware of breathing, and focusing the mind.
There are many styles of yoga ranging from gentle to more vigorous.
What to expect
Wear comfortable clothes. You may be asked to remove your shoes before entering the yoga room. You usually use a yoga mat, which may be provided, or you may need to bring your own. Most classes last about one hour.
A session usually begins with warm-up stretches, followed by a series of yoga postures. A typical routine also involves focusing on quietening the mind and working with the breath, and ends with some form of relaxation.
Laughter yoga combines breathing, clapping and physical laughter exercises. It’s based on laughter as a form of movement and breathwork, rather than anything to do with jokes or humour.
Some cancer centres offer yoga classes designed for people with cancer, having treatment or in recovery.
If possible, see a yoga therapist who works with people who have cancer. This is because certain styles of yoga may not be suitable at some stages of cancer or depending on your abilities.
Ask your yoga teacher about any precautions you should take and possible modifications or support you may need.
Evidence
Clinical practice guidelines on cancer pain include yoga for people with pain related to taking aromatase inhibitors, as well as pain after treatment for some cancers.
They also suggest yoga as a way to manage cancer-related fatigue. There is evidence that yoga can decrease stress and anxiety, reduce sleep disturbances, improve muscle strength and enhance quality of life.
The breathing focus may help reduce pain.
Understanding Complementary Therapies
Download our Understanding Complementary Therapies booklet to learn more.
Download now